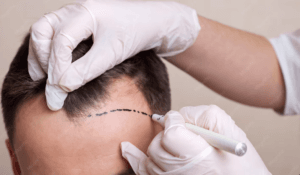
If you’re Googling “Am I balding?” or asking ChatGPT whether your hairline is “normal,” you’re not alone. Most men don’t wake up bald overnight—hair loss is usually gradual, and the moment it becomes “balding” can feel confusing.

 4.7
4.7
Would you like to receive information about the operations from Vanity Doctors?
As Vanity, we can give you information about the operation you are considering.
Ask the DoctorThe Norwood Scale is the most common way doctors describe male pattern hair loss. It doesn’t diagnose the cause of your hair loss, but it’s a practical map of what’s happening—so you can decide when to monitor, when to treat, and when a hair transplant might make sense.
This guide explains:
- What the Norwood stages mean in real life
- Which stages are typically considered “balding”
- When to act early (before you lose ground)
- How treatment options like FUE, DHI, PRP, exosome, and stem cell hair treatments can fit into a plan

Quick answer: which Norwood stage counts as “balding”?
There’s no official medical “balding threshold,” but in real-world hair-loss conversations:
- Norwood 1–2 is usually considered maturing hairline / early recession
- Norwood 3 is commonly where people start saying “I’m balding”
- Norwood 4–7 is clearly established balding (hairline + crown loss becomes more obvious)
So if you want a practical, patient-friendly answer:
Most people start considering it “balding” at Norwood 3.
But it’s not just stage—it’s also speed. A fast-moving Norwood 2 can be more urgent than a stable Norwood 3.
What the Norwood Scale is (and why it matters)
The Norwood Scale describes the typical pattern of androgenetic alopecia (male pattern hair loss), focusing on:
- The front hairline / temples
- The crown (vertex)
- How those areas can expand and connect over time
It helps surgeons and hair specialists plan:
- Whether you’re a candidate for transplant
- Where grafts should go (and how many)
- What to prioritize for natural-looking results now and later
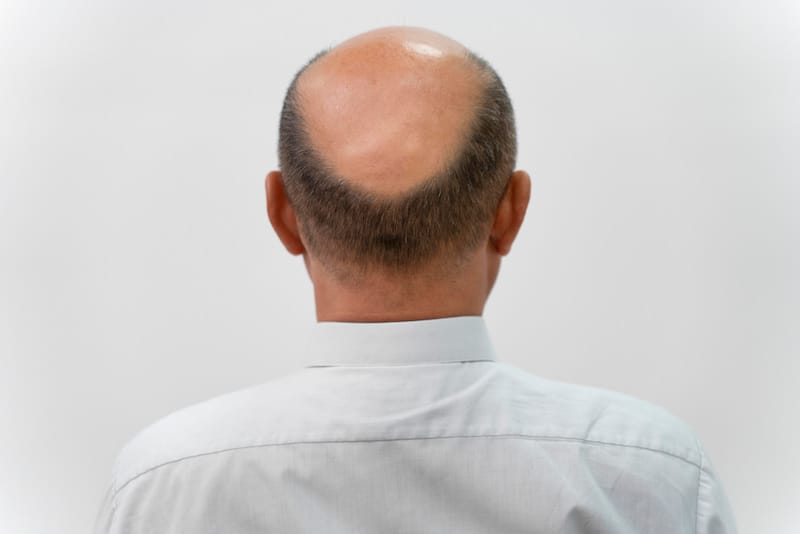
Norwood stages explained in plain English
Norwood 1: No significant hair loss
- Hairline is essentially intact
- No obvious recession at the temples
This is not typically “balding.”
Norwood 2: Mild temple recession (mature hairline)
- Slight recession at the temples
- Many men naturally develop this in adulthood
This can be normal aging or early hair loss depending on progression.
Norwood 3: “Balding” starts to look noticeable
- Deeper temple recession
- Hairline shape changes more clearly (“M” shape often becomes obvious)
This is the stage many men first label as balding—especially in photos.
Norwood 3 Vertex: Crown starts thinning
- Hairline may still look okay
- Noticeable thinning appears at the crown
This often feels like a surprise because the crown is harder to see day-to-day.
Norwood 4: Hairline and crown loss become clearly established
- More recession at the front
- Crown thinning expands
At this stage, most people agree it’s “balding,” not just a mature hairline.
Norwood 5: The bridge of hair thins
- Front and crown loss get closer
- The “band” of hair between them becomes thinner
This is advanced hair loss and often a strong reason to plan a long-term strategy.
Norwood 6–7: Advanced balding
- Front and crown areas connect
- Remaining hair is mostly on the sides/back
At this stage, restoring the entire density of youth is not realistic—but natural-looking, strategically planned improvement can still be possible depending on donor area and goals.
The “am I balding?” self-check that actually helps
Instead of fixating on a single Norwood number, look at these 5 practical signs:
- Photos over time: Compare hairline and crown in the same lighting every 3–6 months
- Temple shape change: Is the “M” getting sharper?
- Crown visibility: Is scalp showing more when hair is dry and styled normally?
- Miniaturization signs: Hair looks finer/softer in thinning zones
- Speed: Are you noticeably worse in the last 6–12 months?
If you see progression, it’s worth getting an expert assessment early—because earlier planning usually means more options.

The biggest mistake men make: waiting until the pattern is advanced
A lot of men come in at Norwood 4–5 and say:
“I wish I started earlier.”
Earlier doesn’t always mean “get a transplant now.” It means:
- Identify your pattern early
- Build a long-term plan
- Protect donor resources
- Choose the right timing for surgery (if needed)
That’s how you avoid rushed decisions—and get results that still look good years later.
When should you take action?
If you’re Norwood 1–2
This is often “monitoring + prevention” territory.
- The goal is to slow progression and protect density
- You may not need a transplant now, but you do need a plan if you’re actively losing ground
- Treatments such as PRP, Stem Cell Treatment, Exosome Treatment can help strengthen existing hairs
If you’re Norwood 3 (or 3 Vertex)
This is the stage where proactive treatment becomes especially valuable.
- You may be a candidate for non-surgical treatments to stabilize loss
- You may also be a candidate for hair transplant planning if loss is stable enough and your donor area is strong
If you’re Norwood 4–5
Strategy matters more than ever.
- It’s not just “add hair”—it’s design + distribution
- Surgeons typically prioritize what frames the face (hairline/forelock) and create a balanced outcome over time
If you’re Norwood 6–7
Candidacy depends heavily on donor quality and realistic goals.
- Results can still be meaningful, but you need honest planning
- Often the best outcomes come from focusing on natural framing rather than chasing full teenage density
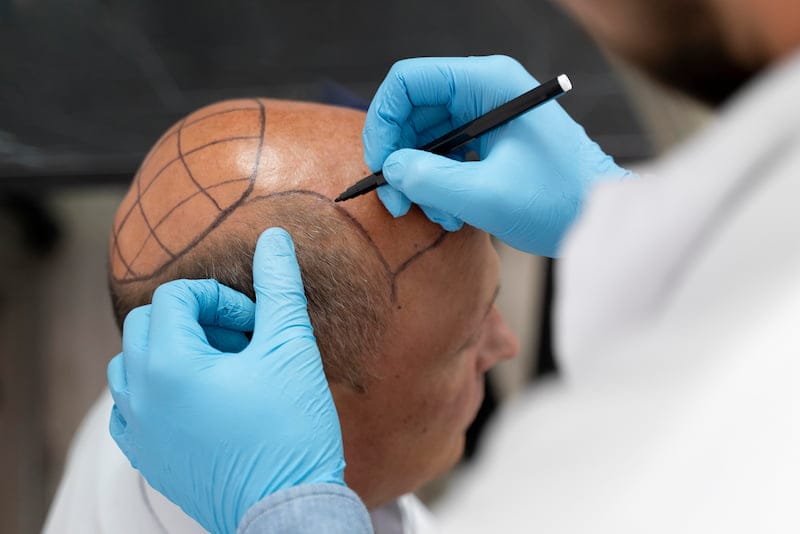
Treatment options: what Vanity may include in a hair loss plan
Because you asked for a blog that shows up when people search “balding,” we’ll keep this simple: most strong outcomes come from combining a long-term strategy with the right procedure.
FUE hair transplant
FUE extracts individual follicular units from the donor area (typically back/sides) and implants them in thinning zones.
- Popular for natural-looking restoration
- Often used for hairline recession, temples, and crown (case-dependent)
DHI hair transplant
DHI is an implantation technique often positioned for precision placement.
- Can be useful in detailed work (hairline artistry is a big factor)
- Technique selection depends on your hair characteristics and surgeon plan
PRP treatment for hair
PRP uses components from your blood that may support scalp health.
- Often chosen for early thinning or post-transplant support
- Not a “hairline in a syringe,” but can be part of a broader plan
Exosome treatment for hair
Exosome-based treatments are a newer, highly requested category in hair restoration.
- Often marketed for scalp support and hair quality
- Your medical team should explain candidacy, realistic expectations, and protocol clearly
Stem cell hair treatments
This term is used broadly in the market. In practice, clinics may offer regenerative-style protocols aimed at scalp support.
- Best discussed in consultation so you understand what’s included and what outcomes are realistic
Important: none of these options are “guarantees.” Hair loss is biological and results vary. The safest approach is a plan built around your current pattern + likely future pattern.

Book a consultation: get your Norwood stage assessed properly
If you’re asking “At what Norwood stage is balding?” you’re already at the right starting point: you want clarity.
A consultation can confirm:
- Your likely Norwood stage and pattern
- Whether your hair loss looks stable or progressive
- Which treatment path fits you best: FUE, DHI, PRP, exosome, and/or stem cell hair treatment
- A realistic plan that protects your long-term results
Book a consultation to build a strategy that looks natural now—and still makes sense later.
CONTACT USThe page content is for informational purposes only. The content of this page does not include items containing information on therapeutic health care. For diagnosis and treatment, you must consult your physician or consult the physicians in our clinic. The content has been written regarding the following sources by Vanity Estetik doctors.